Prematurity, the problem
Being able to detect prematurity in time is the great battle in Maternal-Fetal Medicine
Prematurity * is the leading cause of infant mortality in developed countries, the second around the world, and has an overall prevalence of approximately 10%. In 2016, prematurity represented 35% of deaths in infants and 16% globally in children under 5 years of age. This is one of the most important clinical problems in the world as it is increasing in developed countries. Every year, more than 15 million premature children are born in the world who can suffer complications due to this condition. Prematurity contributes in the long term to suffering disability in the growth and morbidity associated with it, such as cognitive, visual or learning morbidity.
The possible causes of premature birth are very numerous and disparate, being preeclampsia or eclampsia and intrauterine growth restriction the main causes followed by membrane ruptures and pregnancies due to assisted reproduction techniques. The endocrine changes that precede birth in women remain elusive and this makes it difficult to predict spontaneous delivery at term, and much more, spontaneous preterm birth. Early intervention in this group of women would have a significant impact on the neonatal mortality and morbidity figures.
*Defined as a condition suffered by babies born before the 37th week of gestation.
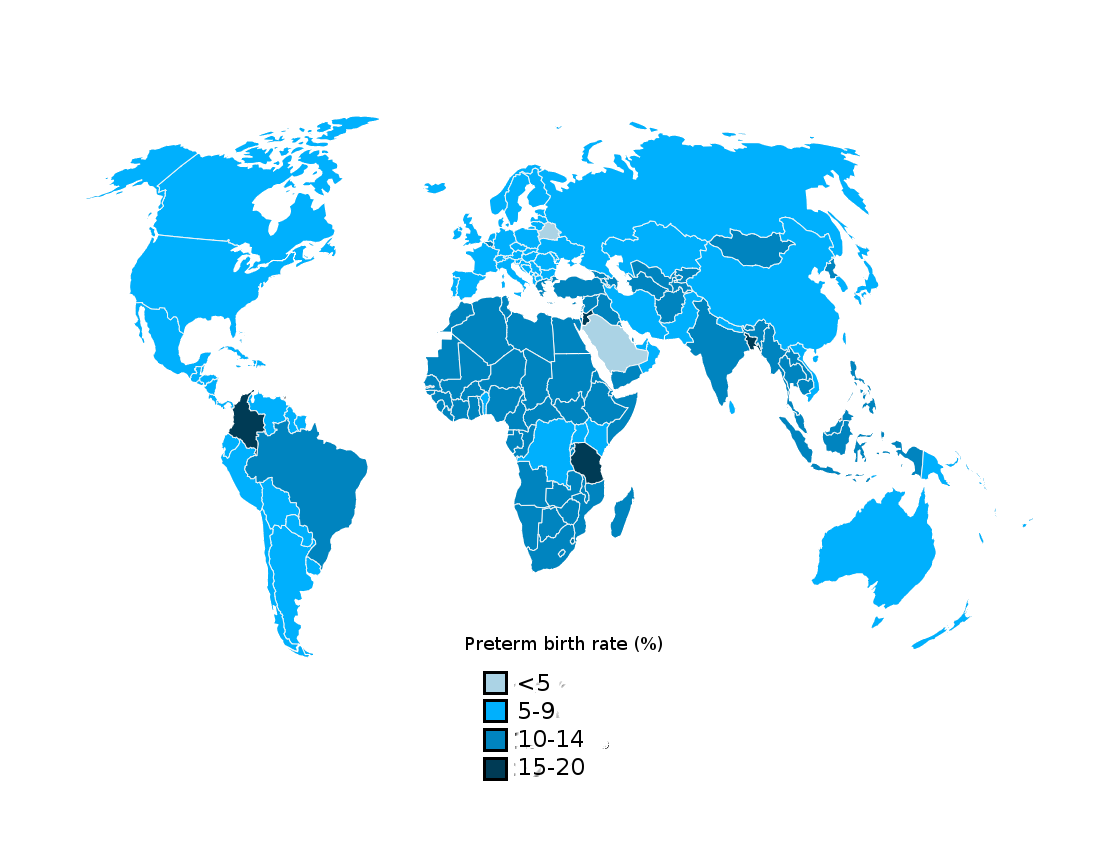
Image adapted from Saifon Chawanpaiboon et als. "Global, regional, and national estimates of levels of preterm birth in 2014: a systematic review and modelling analysis"
Spontaneous preterm delivery the great unknown challenging
More than 50% of cases are due to spontaneous preterm births: unpredictable situations in a routine follow-up of pregnancy, which makes premature birth the most important cause of perinatal mortality and long-term disability in newborns.
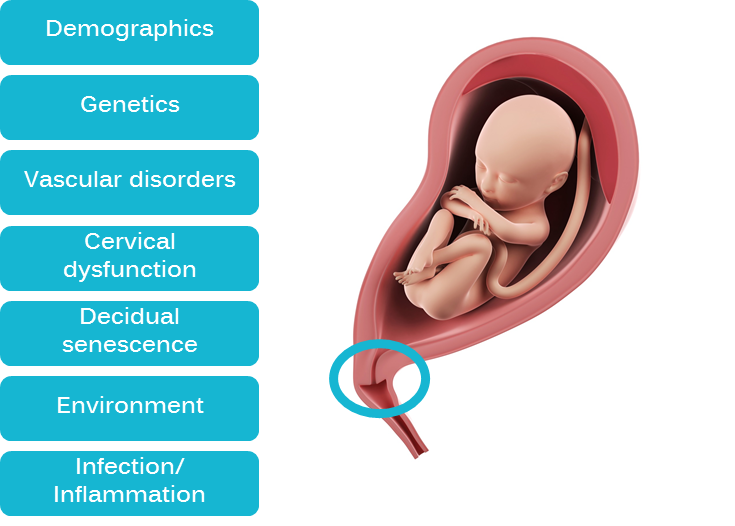
Spontaneous preterm birth is a multifactorial syndrome that can occur through the activation of multiple unknown factors with complex interactions (eg, demographics, infections and inflammation, vascular disorders, cervical dysfunctions). In any case, the activation of an early cervical remodeling always occurs, making the evaluation of the cervix a key element for risk assessment. Cervical remodeling during pregnancy is a chronic process consisting of microstructural changes of the cervix, which begin in the first trimester and end until delivery. The identification of early cervical remodeling could reduce maternal and perinatal complications associated with spontaneous preterm delivery.
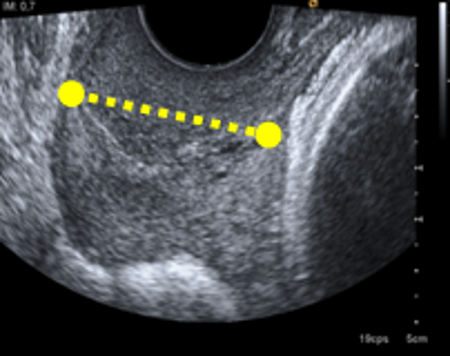
Current techniques: The Cervical Length
The cervical length* is the default method for evaluating cervical remodeling associated with the risk of premature birth. For this reason, reference associations such as ISUOG, SMFM or ACOG mention it as one of the best methods to predict spontaneous preterm birth in specific risk groups, but they do not find it adequate for the general population or as an independent predictor due to its low performance.
The Cervical Length is more reliable than the digital or other tests based on chemical markers, but it still has shortcomings related to its performance due to the great variability in the measurement of cervical length and its low sensitivity, so it is necessary to improve our knowledge of the labor mechanism in women and identify new diagnostic techniques to predict preterm birth effectively.
* Ultrasound technique that is performed transvaginally and allows evaluating the characteristics of the maternal cervix by measuring its length to determine the risk of premature delivery.